Hemorrhoids
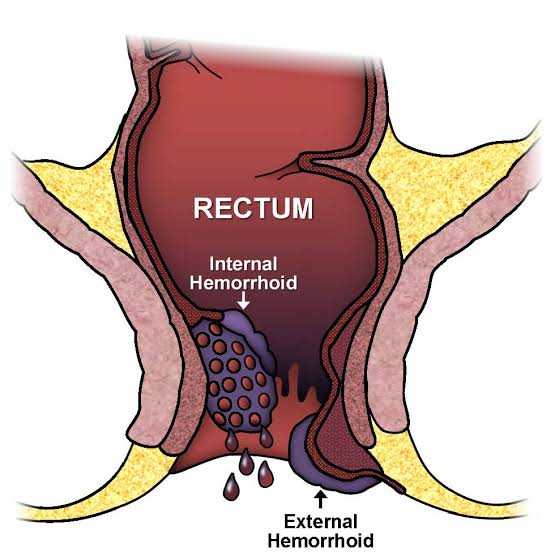
Hemorrhoids (HEM-uh-roids), also called piles, are swollen veins in your anus and lower rectum, similar to varicose veins. Hemorrhoids can develop inside the rectum (internal hemorrhoids) or under the skin around the anus (external hemorrhoids).
Nearly three out of four adults will have hemorrhoids from time to time. Hemorrhoids have a number of causes, but often the cause is unknown.
Fortunately, effective options are available to treat hemorrhoids. Many people get relief with home treatments and lifestyle changes.
Symptoms
Signs and symptoms of hemorrhoids usually depend on the type of hemorrhoid.
External hemorrhoids
These are under the skin around your anus. Signs and symptoms might include:
- Itching or irritation in your anal region
- Pain or discomfort
- Swelling around your anus
- Bleeding
Internal hemorrhoids
Internal hemorrhoids lie inside the rectum. You usually can’t see or feel them, and they rarely cause discomfort. But straining or irritation when passing stool can cause:
- Painless bleeding during bowel movements. You might notice small amounts of bright red blood on your toilet tissue or in the toilet.
- A hemorrhoid to push through the anal opening (prolapsed or protruding hemorrhoid), resulting in pain and irritation
Thrombosed hemorrhoids
If blood pools in an external hemorrhoid and forms a clot (thrombus), it can result in:
- Severe pain
- Swelling
- Inflammation
- A hard lump near your anus
Causes
The veins around your anus tend to stretch under pressure and may bulge or swell. Hemorrhoids can develop from increased pressure in the lower rectum due to:
- Straining during bowel movements
- Sitting for long periods of time on the toilet
- Having chronic diarrhea or constipation
- Being obese
- Being pregnant
- Having anal intercourse
- Eating a low-fiber diet
- Regular heavy lifting
Risk factors
As you age, your risk of hemorrhoids increases. That’s because the tissues that support the veins in your rectum and anus can weaken and stretch. This can also happen when you’re pregnant, because the baby’s weight puts pressure on the anal region.
Complications
Complications of hemorrhoids are rare but include:
- Anemia. Rarely, chronic blood loss from hemorrhoids may cause anemia, in which you don’t have enough healthy red blood cells to carry oxygen to your cells.
- Strangulated hemorrhoid. If the blood supply to an internal hemorrhoid is cut off, the hemorrhoid may be “strangulated,” which can cause extreme pain.
- Blood clot. Occasionally, a clot can form in a hemorrhoid (thrombosed hemorrhoid). Although not dangerous, it can be extremely painful and sometimes needs to be lanced and drained.
Prevention
The best way to prevent hemorrhoids is to keep your stools soft, so they pass easily. To prevent hemorrhoids and reduce symptoms of hemorrhoids, follow these tips:
- Eat high-fiber foods. Eat more fruits, vegetables and whole grains. Doing so softens the stool and increases its bulk, which will help you avoid the straining that can cause hemorrhoids. Add fiber to your diet slowly to avoid problems with gas.
- Drink plenty of fluids. Drink six to eight glasses of water and other liquids (not alcohol) each day to help keep stools soft.
- Consider fiber supplements. Most people don’t get enough of the recommended amount of fiber – 20 to 30 grams a day – in their diet. Studies have shown that over-the-counter fiber supplements, such as psyllium (Metamucil) or methylcellulose (Citrucel), improve overall symptoms and bleeding from hemorrhoids.
- If you use fiber supplements, be sure to drink at least eight glasses of water or other fluids every day. Otherwise, the supplements can cause or worsen constipation.
- Don’t strain. Straining and holding your breath when trying to pass a stool creates greater pressure in the veins in the lower rectum.
- Go as soon as you feel the urge. If you wait to pass a bowel movement and the urge goes away, your stool could dry out and be harder to pass.
- Exercise. Stay active to help prevent constipation and to reduce pressure on veins, which can occur with long periods of standing or sitting. Exercise can also help you lose excess weight that might be contributing to your hemorrhoids.
- Avoid long periods of sitting. Sitting too long, particularly on the toilet, can increase the pressure on the veins in the anus.
Treatment
External hemorrhoidthrombectomy
If a painful blood clot (thrombosis) has formed within an external hemorrhoid, your doctor can remove the hemorrhoid, which can provide prompt relief. This procedure, done under local anesthesia, is most effective if done within 72 hours of developing a clot.
Minimally invasive procedures
Rubber band ligation of hemorrhoid
For persistent bleeding or painful hemorrhoids, your doctor might recommend one of the other minimally invasive procedures available. These treatments can be done in your doctor’s office or other outpatient setting and don’t usually require anesthesia.
- Rubber band ligation. Your doctor places one or two tiny rubber bands around the base of an internal hemorrhoid to cut off its circulation. The hemorrhoid withers and falls off within a week. Hemorrhoid banding can be uncomfortable and cause bleeding, which might begin two to four days after the procedure but is rarely severe. Occasionally, more-serious complications can occur.
- Injection (sclerotherapy). Your doctor injects a chemical solution into the hemorrhoid tissue to shrink it. While the injection causes little or no pain, it might be less effective than rubber band ligation.
- Coagulation (infrared, laser or bipolar). Coagulation techniques use laser or infrared light or heat. They cause small, bleeding internal hemorrhoids to harden and shrivel. Coagulation has few side effects and usually causes little discomfort.
Surgical procedures
- Only a small percentage of people with hemorrhoids require surgery. However, if other procedures haven’t been successful or you have large hemorrhoids, your doctor might recommend one of the following:
- Hemorrhoid removal (hemorrhoidectomy). Choosing one of various techniques, your surgeon removes excessive tissue that causes bleeding. The surgery can be done with local anesthesia combined with sedation, spinal anesthesia or general anesthesia. Hemorrhoidectomy is the most effective and complete way to treat severe orrecurring hemorrhoids. Complications can include temporary difficulty emptying your bladder, which can result in urinary tract infections. This complication occurs mainly after spinal anesthesia. Most people have some pain after the procedure, which medications can relieve. Soaking in a warm bath also might help.
- Hemorrhoid stapling. This procedure, called stapled hemorrhoidopexy, blocks blood flow to hemorrhoidal tissue. It is typically used only for internal hemorrhoids. Stapling generally involves less pain than hemorrhoidectomy and allows for earlier return to regular activities. Compared with hemorrhoidectomy, however, stapling has been associated with a greater risk of recurrence and rectal prolapse, in which part of the rectum protrudes from the anus. Complications can also include bleeding, urinary retention and pain, as well as, rarely, a life-threatening blood infection (sepsis).
